Corrective Exercise: Why Stiffness Can Be a Good Thing
With reference to strength and conditioning programs, the adjective “stiff” is generally perceived to be a bad thing, as folks mean it in a general sense. In other words, you seem “locked up” and don’t move well.
Taken more literally and applied to specific joints, stiffness can be a very good thing. A problem only exists if someone is excessively stiff – especially in relation to adjacent joints. If someone has the right amount of stiffness to prevent movement at a segment when desired, then you would simply say that it’s “stable.” That doesn’t sound too bad, does it?
This is generally a very confusing topic, so I’ll use some examples to illustrate the concept.
Example #1: Reducing kyphosis.
Take your buddy – we’ll call him Lurch – who sits at a desk all day long. He’s got a horrible Quasimodo posture, and he comes to your for help with improving it. You know that his thoracic spine is stuck in flexion and needs to be unlocked, so you’re obviously going to give him some thoracic spine mobility drills. That’s a no brainer.
However, would you say that Lurch would make better progress correcting bad posture with those drills alone, or if he combines those drills with some deadlifting, horizontal pulling strength exercises, and a more extended thoracic spine posture during the day? Of course Lurch would do much better with those additions – but why?
All those additions increased stiffness.
With the thoracic erectors adequately stiff relative to the cervical erectors (which create forward head posture when too stiff) and lumbar erectors (create lordosis when too stiff), there is something to “hold” these changes in place. If you’re just doing the thoracic spine mobilizations, you’re just transiently modifying stiffness (increasing tolerance to stretch) – NOT increasing range of motion!
You know what else is funny? In 99% of cases like this, you’ll also see an improvement in glenohumeral range of motion (both transiently and chronically). Mobilize a thoracic spine and it’s easier to create stiffness in the appropriate scapular stabilizers. When the peri-scapular muscles are adequately stiff, the glenohumeral joint can move more freely. It’s all about understanding the joint-by-joint theory; mobility and stability alternate.
Example #2: The guy who can squat deep with crazy stiff hip flexors.
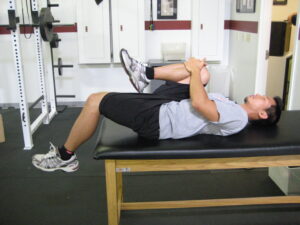
A few years ago, one of our interns demonstrated the single-worst Thomas Test I’ve ever seen. In this assessment, which looks at hip flexor length, a “good” test would have the bottom leg flat on the table with no deviation to the side. In the image below (recreated by another intern), the position observed would be indicative of shortness or stiffness in the rectus femoris and/or psoas (depending on modifying tests):
In the case to which I’m referring, though, our intern was about twice as bad as what you just saw. He might very well have had barnacles growing on his rectus femoris, from what I could tell. But you know what? He stood up right after that test and showed me one of the “crispest” barefoot overhead squats I’ve ever seen.
About an hour later, I watched him front squat 405 to depth with a perfectly neutral spine. So what gives? I mean, there’s no way a guy with hip flexors that stiff (or short) should be able to squat without pitching forward, right?
Wrong. He made up for it with crazy stiffness in his posterior hip musculature and outstanding core stability (adequate stiffness). This stiffness enables him to tap in to hip mobility that you wouldn’t think is there.
Is this a guy that’d still need to focus on tissue length and quality of the hip flexors? Absolutely – because I’d expect him to rip a hole in one of them the second he went to sprint, or he might wind up with anterior knee pain eventually.
Does that mean that squatting isn’t the best thing for him at the time, even if he can’t do it? Not necessarily, as it is a pattern that you don’t want to lose, it’s a key part of him maintaining a training effect, and because you want him to feel what it’s like to squat with less anterior hip stiffness as he works to improve his hip mobility (rather than just throw him into the fire with “new hips” down the road).
These are just two examples; you can actually find examples of “good stiffness” all over the body. So, as you can imagine, this isn’t just limited to corrective exercise programs; it’s also applicable to strength and conditioning programs for healthy individuals. Effective programs implement mobility exercises and self myofascial release to transiently reduce stiffness where it’s excessive, and strength exercises to stiffen segments that are unstable. Effectively, you teach the body how to move correctly – and then load it up to work to make that education permanent.
Want to take the guesswork out of your strength and conditioning programming? Check out Show and Go: High Performance Training to Look, Feel, and Move Better.
Sign-up Today for our FREE Newsletter and receive a deadlift technique tutorial!